Vaginismus Treatment & Symptoms
Maze’s Unique Approach

If sex feels impossible — like your body “shuts the door” the moment penetration is attempted — you’re not alone. Vaginismus is an involuntary tightening of the vaginal muscles during attempted intercourse, pelvic exams, or tampon use, and it can be confusing, frustrating, and isolating. The most important thing to know is this: vaginismus is highly treatable — in every single case, there are options. At Maze Health, we specialize in vaginismus treatment for patients across Westchester, New York City, Connecticut, and New Jersey, combining expert clinical care with a compassionate approach that treats the body’s muscle response while also supporting the emotions that often come with it.
Vaginismus can feel like a betrayal by your own body. You may want intimacy, you may feel safe with your partner, and you may be trying your best — yet penetration still feels blocked by a tightness you can’t control. That’s because vaginismus is not something you “will” to happen. The muscle response is involuntary, and many people don’t even realize it’s the reason intercourse (or even a pelvic exam) becomes painful or impossible.
And while it’s more common than most people think, it’s also deeply underreported. It’s estimated that 7%–16% of women experience vaginismus, but reliable statistics are hard to capture because so many patients struggle quietly, avoid care out of embarrassment, or assume it’s something they simply have to live with. You don’t.
At Maze Health, we want you to hear this clearly: we can help — every single time. Of all pain conditions, vaginismus is one of the most successfully treated, often in a shorter amount of time than patients expect. Treatment may include a structured plan with dilators for gradual, supported progress, or in more severe cases, Vaginismus Treatment Under Anesthesia may be recommended. Either way, every patient meets with one of our therapists — not because “it’s all in your head,” but because anxiety, fear, self-esteem, and body image can become tightly woven into the cycle, and addressing that piece helps your body feel safe enough to change its response.
You deserve a plan that’s clinical, compassionate, and actually works. Maze Health provides specialized vaginismus care for patients throughout Westchester, NYC, Connecticut, and New Jersey. Reach out to schedule a visit and take the first step toward comfortable, confident intimacy.
Vaginismus Symptoms and Diagnosis
Vaginismus is a condition where the vaginal muscles tighten involuntarily during attempted penetration, including intercourse, tampon use, or gynecological exams. This tightening is caused by reflexive contractions of the pelvic floor muscles surrounding the vagina, not by anything a woman is consciously doing. Many patients don’t even realize their muscles are tightening; they only know that penetration feels painful, blocked, or impossible. Vaginismus symptoms can range from burning, stinging, or sharp pain during intercourse to complete inability to have penetration at all. In fact, vaginismus is the leading cause of unconsummated relationships, and its impact often extends far beyond the physical symptoms.

Vaginismus Treatments
The goal of vaginismus treatment is simple: end painful sex and make penetration comfortable again.

At Maze Health, we treat every degree of vaginismus by retraining the pelvic floor and rebuilding confidence step by step — not forcing anything, not rushing, and never blaming the patient. Most treatment plans start with a guided vaginal dilator program designed to relax and re-stretch tight vaginal muscles and rewire the body’s automatic “guarding” response to penetration. Depending on your symptoms and severity, we may also add vaginal medications for muscle relaxation, pelvic floor physical therapy, lubrication support, hormone therapy, or short-term anti-anxiety support. And for severe cases — or when fear makes standard treatment feel impossible — we offer Vaginismus Treatment Under Anesthesia, a highly successful approach pioneered by Peter Pacik, MD, with fast, lasting resolution.
Emotional side of treatment
Treating vaginismus isn’t just about relaxing pelvic floor muscles — it’s also about what happens emotionally when your body finally starts to feel safe again. As patients learn to control spasms, manage pain, and move through treatment, fear often loosens its grip, and sometimes anger shows up instead. Anger that you “have to change,” anger that this took over your life, anger that treatment is work, or anger that you waited so long to get help. At Maze Health, we normalize this completely. Healing from vaginismus can be physical progress and emotional whiplash — and both deserve support.

About Dr. Werner and Maze

About Dr. Werner
About Maze









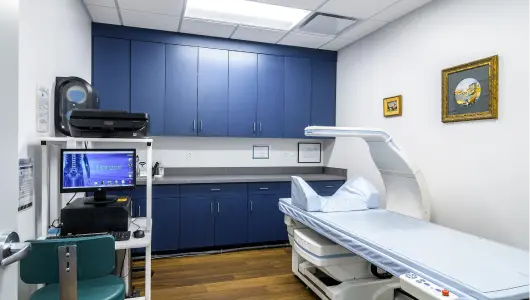
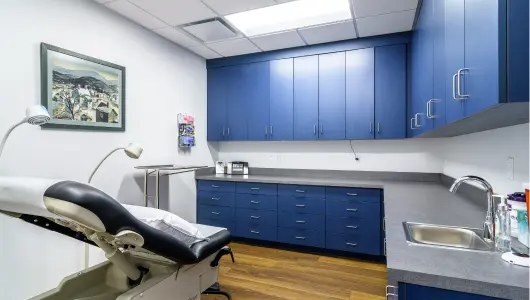







Maze facilities
Areas served
Patient Stories
(Botox Treatment) It seems unreal that I could achieve pain-free intercourse only 51 days post-procedure!
My partner and I planned a trip to Aruba, which was kind of intended to be our honeymoon. Life has felt pretty busy and stressful lately, so we were really looking forward to getting away for some relaxation. We had talked about potentially attempting intercourse at some point during the trip, but didn’t necessarily have any expectations. Then we actually decided to give it a try on the first night and were successful! Since I had dilated with the pink dilator immediately before, insertion was actually relatively easy. Since then, we tried a couple more times. Each time was a slight improvement, but still required very careful movements and communication.
At this time, the whole process still feels a bit like “work” to me, as I need to prep with dilation, and then need a lot of mental focus even during intercourse since I’m getting used to all the new sensations. I know with more experience over time, I will continue to be more comfortable with the feeling, as well as giving up that control. One thing I can say is that it did NOT hurt! And even though it wasn’t the most incredible experience for me physically, we were both overwhelmed with emotion and almost couldn’t believe it finally happened.
When I think about how I suffered from vaginismus for nearly 15 years, it almost seems unreal that I could achieve pain-free intercourse only 51 days post-procedure. Words can’t describe how grateful I am for the staff at Maze. This whole experience has truly been life-changing in the best way. Thank you so much for all your support and guidance along the way.
A, NY, Age 39-
A married couple celebrates a shared victory:
For six and a half years of my marriage, my husband and I felt like we were living under a dark cloud. We were struggling with having intercourse. In fact, we couldn’t have intercourse. I felt embarrassed, ashamed, extremely lonely, and utterly hopeless. And then, I truly believe God sent Tara, Bat Sheva, and Dr. Werner as angels to not only shed light on our situation, but also provide an amazing breakthrough that has changed our marriage forever.
Before going to Maze Women’s Sexual Health earlier this year, I had gone to see an OBGYN and my husband had gone to see a urologist in the second year of our marriage. “Keep on trying” and “Here’s some Viagra and Cialis” were the responses we received. We tried to have intercourse using their advice but were still unsuccessful. We both thought my husband struggled with erectile dysfunction, and when even taking the medicine didn’t help, we were devastated. And as crazy as this sounds, we put this extremely important issue on the backburner until earlier this year.
We knew we couldn’t keep on ignoring this issue so my husband did some research in February of this year and found a YouTube video of Dr. Werner, the doctor on the male fertility side. As we watched, we had a very good feeling about him. After some prayer and discussion, we made an appointment with him for my husband. Fortunately, Dr. Werner wanted to see both of us for the first visit. As we told him our story, he told me that I may also have a problem — Vaginismus. I had never heard of that term before. Apparently, Vaginismus is a condition where there is involuntary tightness of the vagina during attempted intercourse. I knew that my vagina was tight when my husband tried to penetrate, but I always thought if his penis was hard enough, he would have been able to.
Dr. Werner directed me to Maze Women’s Sexual Health that day. I spoke with Bat Sheva Marcus, the clinical director, not only about our current issue, but she also asked about my sexual history. I shared things with her I’ve never shared with anyone. She was so understanding and comforting. Bat Sheva made me feel like my husband and I weren’t alone in our struggle. Already, I felt like the heavy weight that we had been carrying for so long was starting to lift.
After that, I was introduced to Tara Ford, the physician assistant that would help me during the dilation process, a process used to help women overcome Vaginismus. I still remember Tara pulling out this slender, white, plastic stick and telling me that she would insert it into my vagina. I was terrified, but Tara was amazing. She slowly talked me through the whole procedure, never forcing me to do something I wasn’t ready for. And even though there was a bit of pain at first, it wasn’t as bad as I thought. She gave me the tools and tips I needed to try the dilation process at home.
And so, for the next seven weeks, I would meet with Tara and Bat Sheva, almost every week, to continue the dilation process. Tara was my cheerleader, encouraging me and giving me the confidence that I could go to the next level in the dilation process. Bat Sheva would address any questions I had as my husband and I attempted intercourse and made the whole process not so scary. I know this sounds strange, but I actually enjoyed the dilation process. And it’s because of how supportive Tara and Bat Sheva were. There’s no way I would have been able to go through this successfully without them.
After the seventh week, miraculously, my husband and I were able to have intercourse!!! We were both shocked and amazed. All the work that Tara, Bat Sheva, and Dr. Werner paid off!
I think the single most important thing I learned from this whole experience is that I am not alone. Until I went to Maze Women’s Sexual Health, I had felt so isolated. I didn’t realize that so many other women struggled with the same things I did. Tara and Bat Sheva were my community in this struggle and it was so liberating to share freely about this with someone else.
If you are struggling with issues of sexuality, you are not alone. Maze has truly been a Godsend for my husband and I. I cannot say enough about them. And, I am extremely happy to report that we are now enjoying a healthy sex life. I highly recommend coming to Maze. You will be so glad you did!!!
J, NY, Age 42
You and your staff are quite literally the reason that my two precious little boys exist today.
Congratulations on your new book, Dr. Marcus! I am a former Maze (nyc office) patient. I just saw you highlighted on Katie Couric’s Instagram and felt compelled to reach out to you. Your practice changed my life and I will be eternally grateful. Ten years ago I came to you scared and ashamed with a severe case of vaginismus. The Botox treatment and dilation was a lifesaver. You and your staff are quite literally the reason that my two precious little boys exist today. Without the treatment I would most likely still be single, childless and hopelessly unable to do anything about it. Instead, I’m a happy wife, mother, woman! Thank you, thank you, a million times thank you! You do amazing work!!
H, NY, Age 41
How vaginismus treatment under anesthesia treated my vaginismus.
I am 24 years old, and have been living with vaginismus for as long as I can remember, though for the majority of that time I didn’t realize it. I always knew that I felt differently about having sex than many of the people around me as we got older and our sexuality became something that, in our teenage years, my friends and peers became more interested in. When tracing the roots of my vaginismus, I know that my experience with my first boyfriend, when I was 13, is a major factor. He was older than me, and as we became more attached to each other he became more controlling and abusive in physical, emotional, and sexual ways. Being so young and confused it seemed impossible to get away from him, and it very much shaped my early sexual feelings in a way that included fear, guilt, shame, anger, and pain.
During all of my relationships after this I became more interested in being sexual, but without ever having intercourse. I was able to enjoy sexual interactions but always avoided having sex, and never fully explained to my partners why, because I didn’t understand it myself. As I got older I was unable to avoid the fact that we were not having sex, but when I thought about it I imagined a painful and invasive experience that immediately turned me off in every way. My instinct to just avoid sex became involuntary and a reaction that was entangled in my mind as well as my body. I never used tampons, rarely even tried to insert anything inside of me, and avoided doctors appointments that would include this. My first gynecologist appointment that was to include a pap smear was a failure, because the doctor wasn’t able to put even her finger inside of me. Simply being at the doctor’s office and attempting this made me anxious, nauseous, and unable to relax at all. The doctor didn’t tell me anything other than “You just need to learn to relax, or it won’t work” and I always left the appointments feeling like a failure but not knowing why.
When I was 23 this issue came to a head when I started a new relationship and was sick of lying about my issues, hiding them, and constantly obsessing about them. I obsessed every day, endlessly about it. It made me miserable and took a toll on my self-esteem in ways that I couldn’t stand to live with. I finally took the steps and found a therapist who I told the entire truth to, the first time I ever told someone out loud what was going on, which was really the first step because it somehow made it even more real.
After a few months of therapy I found out about the Maze Women’s Sexual Health while researching treatment options for vaginismus online, and heard about the Vaginismus Treatment Under Anesthesia. I read everything I could about it, talked to my doctor about it, and scheduled a phone appointment (since I don’t live in NY). It was very difficult to do, though it seems like such a simple thing. I was afraid and intimidated to face this issue, to keep telling my history to new people, and to take the risk of a procedure I’d never heard about before. After the phone call I had all of the information about the procedure, what would happen, how much it would cost, and felt generally more comfortable with the idea. The doctor I spoke to was almost able to guess my history immediately, the reactions I got from previous doctors, my fears about physical intimacy, and how much of a stress it put on my mind and relationships. She was so positive that I was a great candidate for the procedure and assured me that I should not be afraid, which put my mind at ease more and more. My main concerns that were a factor in my decision were that the procedure would somehow not work, it would be difficult to afford because my insurance didn’t cover it, I would have to travel to get there and spend two nights in NY, and mostly that I was still afraid to have to physically deal with this issue because of how long I had avoided it. Even though I was still very skeptical and unsure I finally decided to commit to going through with it.
The staff at Maze Women’s Sexual Health was very helpful in my decision-making process and went out of their way to assist my financial concerns and finding a place to stay before and after the procedure. I had my pre-op blood test and check-up at my local family doctor and was cleared for the procedure a week before going to NY. My mother and I drove to NY the day before the surgery, and the next morning we went to the surgical center. I was so nervous and still apprehensive about what to expect, though it had been described to me in detail I was still afraid because it was hard for me to imagine how it would feel because I always associated my vagina with nothing but pain.
At the surgical center a nurse from Maze, who I had previously been in contact with and felt comfortable with, got me ready for surgery and helped to keep me calm and relaxed before hand. She gave me a simple external check before the operation and I was sedated. While I was knocked out, there was an incision made in my hymen, I was given a topical anesthetic, medication was injected in my vaginal walls to stop my muscle spasms, which allowed the largest vaginal dilator to be inserted. I was also given a pap smear, which was helpful because I was never able to go through with one without sedation and should have had one years before. When I woke up the nurse was there to help me learn to remove and re-insert the dilators, and I was amazed at being able to do this without pain for the first time in my life. I spent the day recovering with the dilators still in, which was somewhat painful as the sedation and anesthesia wore off, but it was manageable and worth it when I was able to fairly comfortably remove and reinsert the dilators as I needed to. That was the moment when I was finally able to face the fear of something being inside of me, and realize that if I wasn’t afraid of it and didn’t expect it to be painful it was completely manageable. I had a post-op appointment the following day with Melissa where she checked my progress with the dilators and helped me be more comfortable with them, and answered all of the many questions I had about what to do from that point.
In the four weeks since then I have, generally, used the dilators every day and it has gotten easier each time. Two and a half weeks after the procedure I had sex for the first time. It took some patience and preparation, but like using the dilators, it has gotten easier and easier every time after the first. I am currently making the transition from dilating often to having sex often, and I have never felt better or more confident about myself sexually. I have had multiple check-ins by phone and email with the doctors at Maze Women’s Sexual Health and they have been so supportive about my progress. The turning point for me after the procedure was learning to change my thinking, not changing my body physically. When I began to believe that I was capable of adapting to this process, it got rid of my fears about being in pain and gave me the ability to relax my body. For anyone considering this procedure or some type of vaginismus treatment, my best advice would be to consider what you would do about it if you weren’t afraid of your previous perception of the mental and physical pain associated with your body. My answer to that question was that I had to take the risk, and have faith in my ability to allow something new and good to happen in place of the memories of pain and discomfort. It hasn’t been an easy process in any way, but it’s been a completely rewarding one that I am so proud of overcoming.
L, PA, Age 24
It literally felt like he was hitting a wall.
I was a virgin on my wedding night. I was also a virgin the next night and the next and the next. It literally felt like he was hitting a wall. After a few weeks, I sought help from my gynecologist. She gave me three diagnoses (congenital tightness, hypersensitivity, vaginismus), a couple of prescriptions, and a recommendation for a physical therapist. With time, dilators and enough lidocaine, I was able to engage in intercourse sporadically. When the numbing cream wore off, I simply slipped out to the bathroom to bleed and to cry. Though it still hurt, I believed the only way to get better was to keep trying. Again, I tried to explain to someone in my gynecologist’s office. Once they ruled out infection, they had no other explanations. I tried another doctor. She saw no evidence of tearing (then what was bleeding?) and suggested it may be an issue of dryness (but why would a 26-year-old be dry?). She diagnosed it as vulvodynia, and she had the cure, too: Maze.
Maze recognized immediately what my other doctors never saw: the birth control those other doctors prescribed had some adverse effects. Coupled with my natural tightness, it caused painful sex and tearing. Tara and Bat Sheva treated me with hormones and dilation, with patience, humor and frankness.
I cried when Bat Sheva told me I couldn’t attempt sex until I healed. It was such a relief from the crushing guilt I felt. For months I had avoided sex and called myself a coward. I felt guilty for not wanting sex. I didn’t want to face the pain of it, but wasn’t pain the only way to get better? It may not have been my fault that my body was built this way (in fact, it definitely wasn’t), but I thought it was my fault that I wasn’t fixing it. I thought the pain was helping and I was just too weak to face it. I was wrong. Bat Sheva was validating. “Why” she asked “would you do something that hurts you?”
As much as this is a physical issue, it is compounded by fear and guilt. The team at Maze Women’s Sexual health guided and they listened. Even as we cleared away one problem, another would lurk behind it. Each time, Maze had an answer. I’m happy to say that my husband and I have a normal sex life now. It came in waves — ebbs and flows. First, I could tolerate sex. Then the pain went away, but I felt numb (I think what I secretly hoped for was for the pain to be replaced by pleasure). Finally, we found our stride. No pain, no tearing, no fear. Thank you, Maze!
T, CT, Age 26
Vaginismus and dyspareunia after menopause:
Shortly after going through menopause I started experiencing searing pain during intercourse. I spoke to my gynecologist about it and he prescribed some hormone cream. It didn’t help the problem and my doctor said there was nothing he could do. So for many, many years I abstained from intercourse with my husband.
On the Internet one day I found information about Maze Women’s Sexual Health. I was very interested and thought maybe they could help me. I waited four months before I gave them a call.
I called and filled out the necessary forms and set up my first appointment. I first spoke with a sex therapist and then with Melissa. She explained the treatment to me, which was simple enough. During the first treatment I did experience some pain, but worked through it and eventually it subsided. I progressed through the treatment quickly. It took about three months after which my husband and I finally tried to have intercourse again and I was totally pain free! I was so thankful to the Center for their patience and understanding. I am celebrating my 40th wedding anniversary and I feel like a young bride again.
– SS, NY, Age 65 –
SS, NY, Age 65
9 weeks and a return to a normal sex life.
What was the problem?
My problem was that anytime I tried having sex, my vagina simply wouldn’t let anything in. No matter how aroused or ready I was mentally and physically, I would tense up anytime fingers or a penis touched outside my entrance. In the past when I tried having full on intercourse my vagina would feel extremely tight and begin to burn when a penis tried to enter.
How long did you live with it?
The first time I tried having sex I was 17 and did not experience penetration until I was 28, so 11 years.
Did you seek treatment elsewhere? What was that like for you?
No. After refusing to get on the exam table at the gynecologist around age 19, I mentioned to the Doctor that I had heard of a condition called Vaginismus and I thought I may have it. The Doctor told me that only a small percentage of the population had vaginismus and that I did not (with no testing, etc.). That was the last time I went to the gynecologist and avoided the issue with anyone professionally until Maze before my 28th birthday.
What was the cause, if it can be determined or if you have some hypotheses?
When I was 15, I had such bad menstrual cramps that I was sent to the hospital. After this visit, I was sent to the gynecologist to be examined for cysts and given a pap smear. I was nervous to begin with and when the Doctor went to put the speculum inside me, the pain was so great that I became very light headed. I could not and would not allow the Doctor to continue with the examination. The pain that the Doctor put me through triggered my brain and body to associate the touching of the entrance of my vagina to that pain. I had a good grasp on the fact that this experience was the reason that I froze up when a penis got near my vagina entrance but I thought I could fix it myself. Many sexual partners later, I had made no progress besides lots of anal sex.
How did you find us?
Google.
How did you feel about making the call for an appointment; was it a hard thing to do?
When I made the initial call to Maze, I was at my wits end, trying to date guys and not able to have sex with them. I was at a point that I knew I needed professional help and looking back, I believe I was most worried that I would not be able to be fixed or that maybe I had some wild physical condition that required surgery. It was a hard thing for me to finally seek help professionally. Once I made the call though, I knew I was at least on my way to an answer to my problem.
What was your first reaction to your first appointment; did that reaction change over time?
At my first appointment, it was concluded that I did have vaginismus and I could be treated. The Doctor had only placed the smallest dilator on the outside of my vagina. I was too scared to let her go farther but felt I had made so much progress already at that point. After my first appointment, I was mentally focused, ready and willing to start the dilation process and to confront this fear I had. I was nervous, anxious and excited to get the whole thing over with and enjoy my sex life.
How was your condition addressed – briefly describe the treatment?
I used dilators every week and each week dilators got progressively bigger. I knew that some dilatations could take more than a week but I was determined not to let that happen. I thought that if I got sidetracked one week that I wouldn’t be able to get out of my head and that I may get stuck. I stayed extremely focused and did not allow myself to get discouraged if the self-dilations took longer than I would have liked.
How long did it take until the problem began to resolve?
Every week I dilated and moved onto the next size. I started dilations on January 14th and had sex March 21, so about nine weeks.
How do you feel now?
Now I feel great! My sex life is healthy and I now know that my brain and my vagina are on the same page. I am so grateful for the entire staff at MCFS, especially Tara and Bat Sheva for helping me confront my fear.
What is the single most important thing you learned from this experience?
The single most important thing I learned from this experience is that I am a more courageous person than I thought myself to be. Yes, I needed help along the way to confront this fear but ultimately it was up to me to get over the issues I was dealing with and get my brain and my vagina connected.
What would you tell others to encourage them to take action and seek help for their condition?
My words of encouragement are that you must believe in yourself and trust the professionals, that they want to best for you and they know what is best for you. Yes, every dilation is going to be scary but every dilation brings you one step closer to your goal and with every dilation you gain a little more courage for the next time. It may feel embarrassing to take action and get help, but it is absolutely the necessary thing to do.
G, Age 28
Post-menopause treatment:
I was having vaginal pain with intercourse that had developed after menopause.
I probably suffered for a year before I mentioned it to my gynecologist. After trying estrogen locally in various forms and not getting relief, she suggested I call the Center.
I did not call immediately…hoping it would magically go away just as it had started.
Finally I made the call and after reading all the emailed material on sexual malfunction and dysfunction, I felt I was definitely headed in the wrong direction…after all…there was no problem with my sex life…only that it was painful. Hesitantly, I kept my appointment. After spending some time at my first appointment with Barbara and Tara, I was really put at ease and fortunately they felt my problem was simple and could be dealt with quickly.
I’m happy to say after three weeks of using dilators regularly I am back to normal and feeling great.
Sometimes the golden years become a bit tarnished……I should have called sooner to get the sparkle back!!
S, CT, Age 64
Birth after vaginismus:
Last year I gave birth to a healthy little girl…she was actually a VBAC birth with no pain medication!!
I often think back to the first time I came to see you and how painful it was to use those early dilators and how afraid I was then to give birth. It is really amazing how far I have come thanks to all of your help!
In a million years I never would have dreamed that I would be able to give birth without pain medicine! Thank you all so much for all that you did for me!
A, NJ, Age 39
Successful vaginismus treatment changes lives.
Four years ago, I was married and began my sexual life. That’s when my problem started. Every time we tried having intercourse, it didn’t work out. I couldn’t even insert my finger or a tampon into my vagina.
I went to see a hypnotist, a physical therapist and had a special massage, but nothing helped. Everyone told me that the problem was all in my head! Then I heard about Maze Women’s Sexual Health. I called them right away but didn’t make an appointment. I was so afraid that like the previous services I tried, they would not be able to help me. A few months later, I decided enough was enough and called to schedule an appointment.
My husband came with me to the first appointment because I was so nervous and embarrassed by my problem. I thought that I was the only one with such an issue but then I found out that a lot of women experience this.
At Maze Women’s Sexual Health, they explained to me what my problem was and discussed treatment. I started using a small dilator and was surprised that I could actually insert it into my vagina! I continued the exercises every night, going from size extra small to large plus. After 2 months, I was ready for intercourse. I was crying because I couldn’t believe it was finally going to happening.
Maze changed our lives. My husband and I are much closer now.
I want to thank Melissa and Rachel for everything they have done for us. And if you have the same problem, please don’t wait, schedule an appointment. This place is amazing!
I, NY, Age 21
Vaginismus treatment after years of suffering:
I first had sex with a partner at 18, and it was so painful I thought I was going to die. I thought that was normal. It’s your first time, right? Everybody said the first time is painful, that it would get better. It never did. Penetrative sex was always excruciating, as if I was being ripped open from the inside. There was nothing fun or pleasurable about it. I kept waiting for it to start feeling good, but that moment never happened.
I only had one boyfriend in college, and that relationship lasted 3 months. After the first few experiences, I began to avoid men. How could you have a conversation with a potential partner, or even make out with them? You know at some point, sex is going to come up, and you’re going to have a humiliating conversation about how you can’t have sex, and who wants to be with a woman who can’t have sex?
Nobody ever discussed sexuality with me growing up. We discussed the mechanics of it, and birth control, but we never discussed how to feel in touch with our bodies, or how to give and receive pleasure. I thought sex was a natural thing that everybody just inherently knew how to do. My girlfriends told me about the great sex they were having, and people in movies were having sex all the time and enjoying it. I felt like a freak of nature. I couldn’t do something that was supposedly instinct. I felt like a failure as a woman.
I was 23 when I noticed my libido died overnight. I thought maybe I could force it to come back. I tried a lot of one-night stands. It didn’t help with getting aroused, and sex was just as painful as ever. I became depressed and withdrawn.
I started researching “painful sex” on Amazon. I thought, what if I assume that painful sex isn’t normal? Let’s assume the problem isn’t me. Let’s assume it can be solved.I was stunned by the flood of books that came up. Painful sex was apparently an epidemic for women, and I never knew. Nobody ever talked about it. I’d only in the last year begun asking my ob/gyns about this. Every doctor said the same thing, “I don’t know. Maybe you just haven’t found the right partner yet.” This always made me want to scream.
I immediately googled clinics that treated painful sex and I couldn’t believe my luck when I discovered Maze Women’s Sexual Health. I made an appointment for the following week.
The waiting room staff was just as friendly in person as they were over the phone, and I was relieved to see it was all women. My team was Melissa (a Family Nurse Practioner) and Rachel (a Clinical Psychotherapist). I was pleasantly surprised by that. It was obvious that Maze cared about physical as well as mental and emotional health. They wanted to tackle my issue from all angles. I felt comfortable right away. I think that first session, I just spent 45 minutes talking Rachel’s ear off about my sexual and relationship history. Rachel was fantastic. She listened, didn’t judge, and just held the space for me while I unloaded at least 12 years of feelings.
I was a little scared going into an examination room with Melissa. Going for my yearly ob/gyn check-ups was always traumatic because I couldn’t stand being touched. Melissa was super understanding, though. She used a child-size speculum and gave me a mirror so I could see what she was doing. That took away a lot of the fear. Melissa discovered that my vaginal muscles were super tight. She said I’d probably had a tight pelvic floor since childhood and just never realized it. Treatment included loosening my muscles with dilators and a referral to a local physical therapist. I was relieved.
Melissa also did a full work-up on me: blood, hormones, the works. I was shocked to find everything come back normal. There was nothing wrong with my body, aside from a tight pelvic floor, which was fixable. At home, I continued working with the dilators. I went at my own pace and controlled use of the dilator, and with daily practice, I grew more and more comfortable feeling something inside me. As the strength in my pelvic floor increased, I began to use bigger dilators until I was at the biggest size, which I NEVER EVER thought was possible.
My mom noticed a change in me the day of my first appointment with Melissa and Rachel. I worked with Maze and my PT for over a month. Now, after only two months, I feel connected to my body, to my inner being. I feel like a woman.
If you’re having issues with your sexual health, don’t wait. I waited for years because I didn’t think there were any other options. I thought living with pain was normal. It’s not. Women and girls are rarely taught about how to have a healthy sexuality, so we don’t even know how to react when we have a problem. I lived with painful sex and depression for 12 years, and I didn’t have to. The team at Maze is amazing and they’re here for you.
CA, NY, Age 30
Vaginismus treatment success story:
Sex was very painful. For some reason (which ended up being vaginismus), I could not have sex without pain. I didn’t know why, but it lasted for over a year before I sought help. It was emotionally, psychologically, and physically hard to deal with; I didn’t want to talk to anyone (other than my husband) about it. Part of me thought it would get better. Part of me was afraid to talk to my doctor about it. Part of me felt embarrassed-why couldn’t I do something that everyone else could? I didn’t even know how to go about addressing it. I felt like the problem was so big — I didn’t know where to begin or what to do.
I finally went to my gynecologist who referred me to the Maze Women’s Sexual Health.
I was very afraid to make the first call. I probably cried for like 20 minutes before I dialed. I didn’t want to talk about this. I had lots of questions and was scared I would cry when I asked them. The woman I spoke to was so calm, helpful, and reassuring. I couldn’t believe how much calmer I felt just after the first phone call.
I was kind of a wreck the day of my first appointment. I was so nervous — partly to talk about this and partly for any exam I might have. I met with Bat Sheva who was the most reassuring person I have ever met. She listened to me and within minutes I knew I was talking to someone who really understood and was going to help me. I then met with Tara for my exam who is the most awesome person. She managed to make me laugh and made me feel so calm. Bat Sheva and Tara helped me feel in control and “normal.” They explained everything to me, understood every question I had, and patiently answered the same ones over and over. They made me feel like I had a team on my side.
I started with the dilation at my first appointment. I went up a size (and sometimes 2 sizes) every week. I had never thought that I would be able to do that. I was actually proud of myself.
It took me less than 2 months for my treatment to work! Within that short time, I got used to the dilation, and intercourse has not been painful. It is such a change. I am so grateful. I am still maintaining the dilation and I feel much more comfortable and in control of my body. I feel proud and happy that an issue that was so hard for me for over a year was able to be solved in less than 2 months.
This experience has taught me to not be afraid to ask for help. I was able to work with the most amazing people who were able to give me all the support I needed. I felt very alone dealing with this issue for over a year. From my first appointment, they became my support team.
When I was first referred here, I remember reading the other testimonials. They made me feel better- like I wasn’t alone. At the same time, I had this worry that I would be the exception; that my issue somehow wouldn’t get fixed; that I would be different. Within minutes of my first visit, I was reassured over and over that I wasn’t the exception; that there was a solution; that I really wasn’t the only one. I think its normal and, of course, understandable to feel that way — to feel scared. From someone who was there, I understand and I encourage you to seek help. With the right people on your side, you won’t believe how fixable this is. I still can’t believe it, but my life has changed. Everyone deserves that.
E, NY, Age 25
Terrified of penetration:
I always knew I had a unique situation/problem because the thought of inserting a tampon or anything else in my vagina terrified me. Before finding the Maze, I tried going to a psychiatrist and even a gynecologist to discuss my fears in addition to my fear of intercourse.
During my first visit to the gynecologist, she insisted on doing a pap smear, which terrified me as well. When she then insisted on only inserting her finger, she was amazed at how nervous it made me and sent me home. Her only advice was for me to seek a therapist, and she made me feel like I had a severe, abnormal problem.
I felt really hopeless, and I began researching different therapists.
As I was searching the internet, I came across the Maze and decided to call them right away. From the first phone call, I really felt that the staff understood what I was going through and assured me that I wasn’t alone and that they have successfully treated so many women with the same problem.
Upon my first visit, I was diagnosed with vaginismus. I began seeing Barbara once a week for therapy and I began the dilation process with Tara. They really made me feel comfortable and didn’t push me to do anything I wasn’t ready for. After 4 months of treatment, I was able to have intercourse without anxiety or fear. I was also able to successfully have a pap smear and the thought of tampons isn’t distressing!
I truly feel liberated and now able to have a healthy and enjoyable sex life. If you are struggling with any of the symptoms I described above, don’t hesitate to call the Maze. They are amazing at what they do!
F, NJ, Age 29
Overcoming the pain and anxiety from vaginismus:
Due to the sensitivity at the opening of my vagina and the tight muscles all around, I had painful intercourse. I lived with the pain for about half a year thinking it would go away. When it didn’t, an expert directed me to Maze Women’s Sexual Health for help.
Getting through to the Center (and scheduling appointments) was pretty easy and the people
I dealt with were extremely kind and accommodating!
At first, I was really uneasy about my visits since whatever was done to determine the problem caused real pain and irritation. Thanks to the support of Bat Sheva Marcus and Tara Ford, I learned to bear the pain and do what was necessary. I started doing dilation exercises every day for 10 minutes, changing to a bigger sized dilator every week. I was quite skeptical about what the results would be, but thankfully with time I felt a real difference and I became more comfortable with the entire dilation process.
It’s about two months later now and thank goodness my sex life has been great and totally different. I no longer have to fear pain, irritation or anxiety. I’m maintaining my dilation exercise for now and hopefully I’ll be totally done with it pretty soon.
This experience showed me that with determination, support and positivity everything is possible! You just need to do the right thing and go to the right places for help.
THANK YOU Bat Sheva, Tara and everyone else at Maze!!
CG, CT, Age 20
Successfully treating vaginismus:
I became sexually active when I got married and intercourse was extremely painful from the beginning. I tried to seek help from my practitioner who advised me to read books on female sexuality and to practice kegels as often as possible. Two years of doing kegel exercises seemed to help a little (i.e. made intercourse ‘bearable’), but after delivering my first baby everything went downhill. Postpartum sex was basically impossible because of pain and vaginal tightening. After trying a few treatments my OB sent me to an Urogynecologist who tried numerous procedures including local anesthesia shots, before finally recommending Maze Women’s Sexual Health.
By the time I contacted the Center I was nervous that this was my last resort at a functional sex life, and I was terrified that if they couldn’t fix my problem I would be out of options. I was initially skeptical of the dilation and therapy visits but as time wore on, the pain began to lessen and I was able to dilate using the largest dilators. During the therapy sessions the doctors clarified what might be viewed as ‘normal expectations’ in a person’s sex life, and taught me to embrace non-intercourse sex as well.
After two months of daily dilation I was ready to try intercourse, and I was shocked when there was virtually no pain. I cried from happiness when I realized that my sex life could be normal and healthy. I still cannot believe how far we’ve come.
Thanks to Maze I now think about sex and intercourse in a different, healthier way. I also feel equipped to deal with vaginismus problems, should they relapse. It’s also great to know that I can always call Maze with any problems or issues that might come up.
I cannot stress enough how important going to Maze was for me. They made me feel comfortable and empowered to do something about my problem, and my marriage as a whole is so much better because of them.
If you think you have a problem with intercourse PLEASE seek help. Nobody should have to suffer through intercourse pain; these problems are common, and incredibly treatable – if you get the right kind of help.
Maze – thank you!
RW, NY, Age 29
Gaining a healthy sex life In two months:
For over a decade, I suffered in silence about my inability to have sex. Because I grew up in a religious family, it wasn’t something I could ask for help with, nor did I connect with a doctor whom I felt comfortable discussing my problems with. I felt unwomanly and even less than a human being. My self-esteem was so low, I put my head down in social situations and avoided going out and meeting people in general. All of my romantic relationships ended because of the situation. One day I mustered up the courage to call Maze Women’s Sexual Health. Within two months my psychological and physical issues were remedied and now I am able to have a normal, healthy sex life. The counselors and medical professionals are extremely thoughtful, understanding, and gentle. I would recommend to any one suffering with a sexual disorder to call Maze. They will change your life.
J, NY, Age 31
Vaginismus treatment cured fear of penetration:
Once I reached 40 years old, I knew I needed to take care of my health and start to have regular pap smears, but I was avoiding it because I had a fear of penetration. I also had an aversion to female genitals. I seldom looked at my own and could only be touched either by myself or my partner with a soft fabric, or vibrator. Luckily I was able to have orgasms very easily and my boyfriends where always fun, kind and affectionate.
Coming from the UK, I had the opportunity to be working in New York City for 12 weeks, and I was determined to get help for my problem (which I now know is called Vaginismus). I was both excited and nervous when I found the very informative website www.mazewomenshealth.com, and that they had a New York City location.
My first action was to get the information pack via the website. I then read everything about Maze including available treatments and the testimonial from other patients. I knew this was ideal for me…I was going to call Maze, but due to the location I decided to just go to the office. Making the first move can often be the most difficult part, so I decided to “just do it”.
In the office I met Johanna at the front desk who was both friendly and informative. She explained the procedure for new patients to me and went over cost of treatment, as well as Maze’s credit system for those not covered by insurance. I left feeling a sense of relief.
My first appointment a week later was with Bat Sheva Marcus. She was very warm and open. I was a little nervous and was talking a lot, but she allowed me to talk and was very kind in her replies. She reassured me that I was not alone, and I was going to get all the help I needed. Talking to someone about your sex life and personal issues is nothing to be embarrassed about or to feel shameful over, and with her soft-spoken way and professional approach she made my meeting feel like I was talking to a good friend. Our conversation covered many topics and I realized she needed to get to the physiological root of my problem. I found I was a little tearful having never spoken to anyone about it before, but thankfully was able to laugh a little too.
My next meeting across the hall was with the caring, smiling Physician Assistant Tara Ford, who was there to examine me.
Tara talked me through the physical. She gave me as much time as I needed and explained Vaginismus to me and started me on my treatment of dilators…..my homework was to use the dilators every day for a week and then come back and move on to the next size.
I had a few difficult days while trying to do my daily dilators but I did not miss a day and only ever had a mild stretching sensation and never experienced any pain. I was also a little teary at times which Bat Sheva explained can happen due to regret or sadness about the loss of time. I was prescribed an estrogen cream as well for dryness.
In just over a month I was feeling more connected to my body! I was reading books on sex, male and female anatomy, and bought a large mirror so I could look at my genitals. I was getting more and more relaxed.
Each week I would talk with both Tara and Bat Sheva and learned more about various lubes and vibrators and my plan for eventually having intercourse. All in all I found my experience at Maze to be really positive, and urge other woman not to be afraid. Don’t let years go by without getting help. You owe it to yourself and your partner to enjoy a satisfying love life!
C, NJ, Age 47
Dealing with vaginismus:
Since getting my period at the age of 12, every time I tried to use a tampon I couldn’t get it in. Eventually I gave up. I felt awkward asking my mom about it, so I never talked with her. When I was a little older, a friend told me that tampons hurt her until she lost her virginity, and then they didn’t. I thought maybe this would be the case for me. My mother never took me to get a pelvic exam, and I didn’t date in high school, so I didn’t realize what a serious issue I had until college.
At 21 I began dating my first serious boyfriend, and decided I wanted to lose my virginity to him. We tried, and he could not penetrate me. Very frustrated, I talked to my friends and they thought that maybe I was just nervous. I went to my college health center to get on birth control and to get my first exam, and the nurse could not perform the exam as it was extremely painful, I started crying and she stopped. She suggested I see a “real” gynecologist. She thought maybe I needed to get my hymen cut…I went to a gynecologist, (for the first time) and I cried when she inserted her finger in me. She said everything “seemed fine” and gave me a brochure for Maze. That year was my senior year of college, and I was very busy. I kept putting off going, making a thousand excuses for why it wasn’t the right time for me to go.
After I graduated college, I didn’t have medical insurance. A year and half went by, and I finally got a job with health benefits- I knew I had to go. I would continually go back to the Maze website, and I knew I had vaginismus. At that point I was single, but I knew I wanted to deal with my vaginismus so that I could eventually have a healthy sex life.
I called the office to make an appointment, only to find out that my insurance didn’t cover ANYTHING! I decided to pay out of pocket, knowing that my health and happiness are far more important than any amount of money.
My doctors made me feel very at ease. It was amazing to describe my experiences and have them nod their heads, yep- vaginismus. I thought, oh, other people go through this? I’m not such a freak after all! We started with dilation, as I felt this was a more natural approach than the Vaginismus Treatment Under Anesthesia. My doctors were very sweet and patient with me. We started on the smallest size, which was extremely painful. The first few appointments I cried every time she inserted the dilator. But then I would go home, and in the privacy of my bedroom I could relax, do my “homework” and each week started to feel better. I would move up a size each week (or 2).
During this time, I had begun dating a great guy. After we were together for a month or so I explained my condition to him. He was very understanding and patient. After 3-4 months of treatment, we had sex. The next few months were up and down. Things were good, but then I went on a birth control that gave me crazy mood swings and made me very dry. I stopped dilating and would have sex like once a week, which made things painful. I was still checking in with my doctors every 4-6 weeks, but began to go more regularly again. We decided that I should go off birth control, and rely on condoms. Going back to regular dilation and not being on birth control pills made sex pain-free again.
Over a year later, I am still dealing with my vaginismus. If I don’t have sex for a few days, I remind myself I HAVE to dilate in order to continue to have a pain free sex life. I had this idea that I would be walking off into the sunset, which isn’t what happened, but that’s real life. I cannot stress to you how important this experience has been for me. I seriously thought I would never have a pain free sex life. I am so blessed with a wonderful boyfriend who went on this journey with me. Sex went from painful, to neutral, to GOOD.
I want to stress that this is a MEDICAL CONDITION: it is not your fault, and it is something that must be treated. Regardless of your relationship status, financial situation, or religious affiliation, I encourage you to seek treatment. You will feel incredibly empowered.
”Do not let your fire go out, spark by irreplaceable spark, in the hopeless swamps of the approximate, the not-quite, the not-yet, the not-at-all. Do not let the hero in your soul perish, in lonely frustration for the life you deserved, but have never been able to reach. Check your road and the nature of your battle. The world you desired can be won. It exists, it is real, it is possible, it is yours”.
Good luck on your journey.
– C, NY, Age 24 –
C, NY, Age 24
Vaginismus treatment under anesthesia and dialation combination treatment:
I got married in May 2010. I had a very interesting sexual relationship with my partner before getting married, but we never tried to have intercourse. During our honeymoon, we tried a lot of times to have intercourse, but failed terribly. Things deteriorated every time we got in bed as it started to feel like trying execute a mission which always fails, so we stopped trying so hard. After 6 months or so, I visited two gynecologists. One of them refereed me to a therapist who introduced me to the idea of dilation. We started with the smallest size which went fine, but then she gave me the bigger size which I could not dilate with. By this time she had identified me as a vaginismus patient. My husband started searching online for causes and treatments, and he found Maze Women’s Sexual Health and Vaginismus Treatment Under Anesthesia. First it sounded scary, but at the time I had no other options. I was losing all my self-confidence and I felt like a freak that could not open her legs to anything, not even for a medical exam or even inserting a tampon!
I went there for the first appointment, where I met with amazing doctors. They were very friendly and very professional and they identified me as a vaginismus patient as well, and offered me two kinds of solutions – one was continuous dilation and the other was the Vaginismus Treatment Under Anesthesia (which I originally called to ask about). They explained the procedure to me, and four months later I scheduled and had the surgery which went very smoothly. After the procedure I started dilating with larger sizes of dilators which I never imagined I would be able to do! The led to having successful intercourse.
It took my husband and I a lot of research and courage to be able to do this since I live in a country where no one has ever even heard of the Vaginismus Treatment Under Anesthesia. I know it sounds like a cliché, but seriously, Maze Women’s Sexual Health changed my life. I am finally a normal woman and my relationship with my husband went back to magnificent again.
Finally, I just want to thank all the Doctors at Maze, everyone I met has been a great help and they are all really comfortable people to talk with. I felt at ease the moment I stepped into Maze for my first appointment up to this moment. Special thanks to Melissa who has been supportive all the way and amazingly friendly.
N, NY, Age 29
Cured my vaginismus and gave me the confidence to meet my boyfriend.
I was a virgin when I started treatment at Maze Women’s Sexual Health.
I had always been anxious about vaginal penetration and had also had some painful gynecological exams. My gynecologist said my hymen was especially thick, so I had it surgically removed. When I still wasn’t able to insert a tampon or anything else months after the surgery, I knew I needed help.
I went to Maze and worked with Melissa for a couple months, practicing with dilators. Each week I graduated to a bigger dilator. By the end of the treatment, I was able to successfully have (pain-free) sex with a male friend of mine. A few months later, I met a guy from an online dating site who lived out of state about two hours away. We’ve now been together 5 months and are are very happy.
Working with Melissa got me through something that felt impossible at the time. I probably would have been able to conquer it on my own eventually, but not without a lot of pain…not just physical, but emotional.
I’m also pretty sure I wouldn’t have had the confidence to meet my boyfriend if I hadn’t felt sure my vaginismus was cured. I’m very glad that I went to Maze Women’s Sexual Health.
– B, NY, Age 26 –
B, NY, Age 26
Frequently Asked Questions
What causes Vaginismus? Is it caused by sexual abuse?
What is the best form of treatment? Is there a permanent cure?
Are there resources available for my spouse/partner?
Can vaginismus miraculously disappear?
What is the best way to incorporate your partner into your treatment?
What are ways to conquer avoidance? / How can I get over my avoidance of sex?
It is so difficult to come face to face with Vaginismus. By educating yourself and knowing that you are not suffering alone you are better able to accept the diagnosis. I think it is vital to be kind to yourself and not judge.
Once patients are aware of the many other patients who are managing Vaginismus, they then feel empowered to seek help. Questioning then accepting are the very first steps in overcoming Vaginismus.
One can easily avoid sex when they are suffering from Vaginismus. There are many other types of intimacy that do not involve intercourse. I think that becoming a sexual person starts with the self. Masturbating and using vibrators can be both pleasurable and help while going through the treatment of Vaginismus. Eventually you can transition from self to partnered sex when you feel comfortable doing so.
What are a woman's options when vaginismus is impeding her ability to get pregnant?
“Pregnancy and Vaginismus” is a topic we regularly receive questions about here at Maze. I think it is vital to overcome vaginismus before attempting pregnancy if this is an option for you. Pregnancy involves multiple trips to the obstetrician to assess both maternal and fetal well-being. Although some visits do not involve internal exams as the obstetrician is just listening to the baby’s heartbeat, measuring maternal vital signs, and measuring the size of the uterus to make sure the baby is growing well, many visits do.
In the beginning of pregnancy, an internal vaginal sonogram is standard in order to measure size and dates to confirm a due date and to check for fetal viability. If you have vaginismus, this internal sonogram can be difficult and potentially cause a good deal of pain and emotional trauma.
As patients head into the last few weeks of their pregnancy, weekly internal exams are sometimes necessary to check for cervical dilation and fetal position.
If Vaginismus is impeding your ability to get pregnant, you can opt for IVF or IUI but these are still difficult to do and very costly.
How does Vaginismus affect child birth and delivery?
Can vaginismus be hereditary?
Is vaginismus a form of anxiety?
Vaginismus is not a form of anxiety. It is defined as the involuntary tightening of vaginal muscles. With that being said, many patients with Vaginismus do suffer from some form of anxiety. Whether the Vaginismus has caused the anxiety is often discussed.
At Maze our patients have a very thorough psychosocial intake before meeting with the medical providers. Patients can have a history of sexual and emotional abuse in conjunction with Vaginismus.
The majority of our patients present without any history of abuse and just have tight muscles which causes Vaginismus.
Any tips for having sex for the first time post-treatment?
Sex for the first time can be both exciting and scary. We suggest dilating before having intercourse.
We also recommend 2 positions for the first few attempts because they simulate the insertion of dilators. Lie on the bed with your legs apart and your feet propped up on chairs with your partner standing between your legs. Have your partner insert the largest dilator so that he can adequately gauge the appropriate angle. Then using his or your hands, slowly insert his penis into your vagina.
Another position is the missionary position. Have your partner kneel between your legs as you are lying on your back. Again have your partner insert the largest dilator so he can adequately gauge the appropriate angle. Then using his or your hands insert his penis.
Once your partner is fully inside and you are relaxed enough and you are not experiencing any pain, let him start to move slowly and gently.
Remember to use adequate lubricant to make insertion easier.
Are there any treatments for severe life-long Vaginismus?
At Maze, we treat every degree of vaginismus. We begin with a gentle dilation program. We often prescribe vaginal muscle relaxant suppositories to help relax tight muscles and we offer a ton of encouragement every step of the way.
If we are not successful with dilation we do offer Vaginismus Treatment Under Anesthesia. You are not alone and we can help you.
Are there birth control options for women with vaginismus that do not require pap smears how do other women handle this when it is traumatic to have a pap smear. How do you have that conversation with a doctor?
There are birth control that are available to you that do not involve a pap smear. Your age determines whether or not a pap smear is necessary.
The only form of birth control which could be difficult for a patient with uncured vaginismus is an IUD as it needs to be inserted into the uterus in your gynecologist’s office.
As far as birth control, there are many options. You can take birth control pills, get the depoprovera shot, use the orthoevra patch, or use male or female condoms. Condoms prevent Sexually transmitted diseases and do not require a prescription.
In terms of discussing Vaginismus with your Gynecologist, this can be tricky as many gynecologists do not know how to counsel women regarding Vaginismus.
I suggest finding a gynecologist who does treat female sexual dysfunction. These gynecologists are generally well versed in vaginismus and can see you through a pap smear. If you are already dilating, I suggest dilating before the gynecology visit and Pap smear.
Why do Doctors and Gyn's ignore vaginismus? Why is the medical community so insensitive to vaginismus sufferers?
Many gynecologists are not trained in vaginismus during both medical school and residency. This is a major problem in terms of the training that they receive. We are hopeful that this will change in the near future as Vaginismus is no longer a condition that is not talked about by both the media and by patients themselves.
